
While not a solution to the maternal health crisis, good communication can help expectant patients feel safe getting care during COVID-19.
Read More
All industries need translators and interpreters who are trained in […]
Read More
Caring for his dying patient, a much-loved Irish farmer with advanced renal failure reminded a doctor of what’s really important in medicine.
Read More
What should you do when you notice your doctor is distracted? A primary care doctor provides tips to help them get back on track.
Read More
Although compassion and empathy are innate qualities, specific education and training can sharpen and improve how physicians deliver bad news to patients.
Read More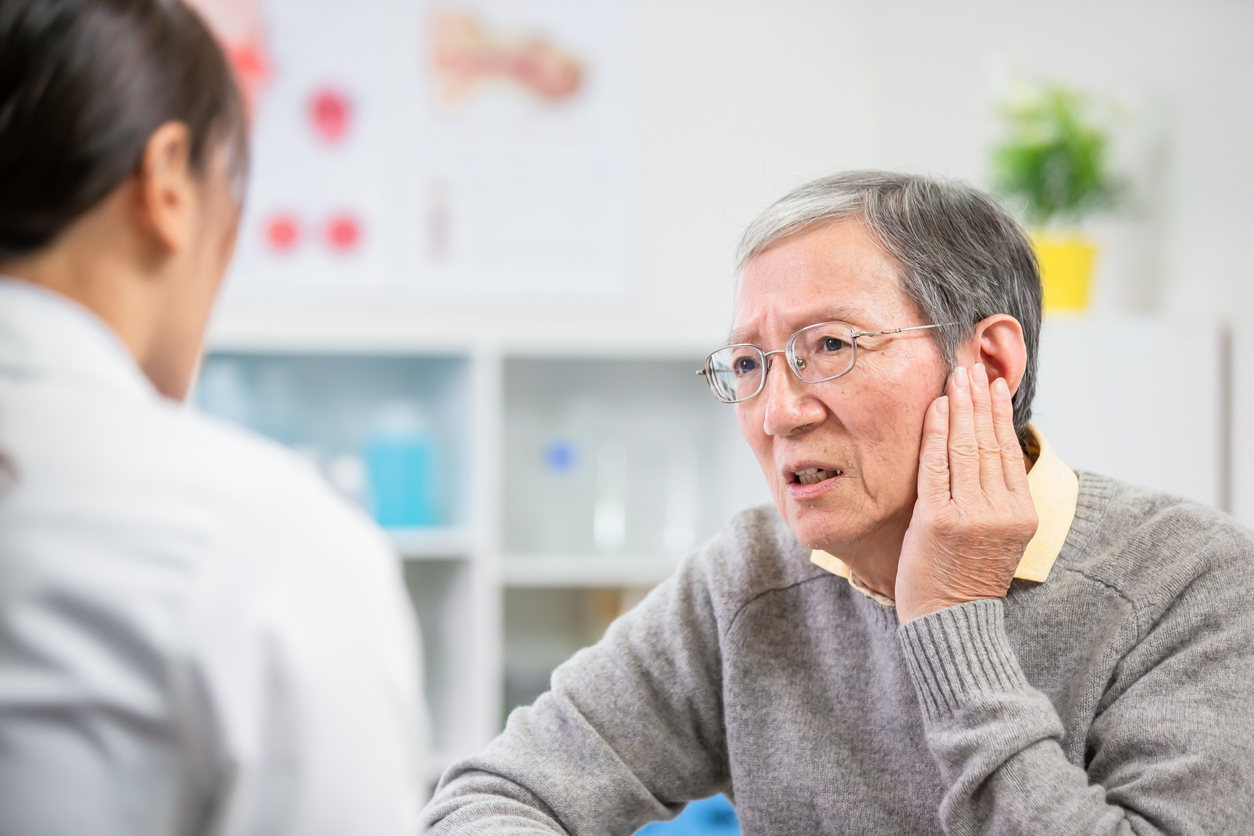
Individuals and their caregivers are the greatest untapped sources of information, knowledge, and motivation
Read More
Doctors working in the field of women’s health should be prepared to listen to all concerns presented by patients & take a holistic approach to their care.
Read More
A new survey shows us that patients have a strong desire for their physicians to be involved in helping them with chronic illness management self-care.
Read More
A new care model, the multidisciplinary specialist team, has the potential to improve patient care and allow physicians to grow personally and professionally.
Read More
Patient engagement has emerged as a key component of reducing the likelihood of an adverse outcome – both clinical and medicolegal.
Read More
Is your doctor overwhelmed by patients and other clinical duties? Here are some things you, as a patient, can do get your doctor to truly engage with you as a person.
Read More
A recent study confirmed that doctors who use positive language reduce patient pain by a similar amount to drugs. Other trials show that positive messages have numerous benefits, ranging from helping Parkinson’s patients move their hands faster to reducing how much pain medication patients use.
Read More