Regardless of your chronic condition, keeping it as well-controlled as possible — meaning low disease activity or remission — is the goal.
Read More
Comprehensive eye exams do more than check if you need new glasses. They also include tests for eye diseases. And, they may detect some chronic diseases.
Read More
Induced pluripotent stem cells (iPSCs) are important tools in many areas of cardiac research including disease modeling, drug development & transplantation.
Read More
There is no single factor that causes addiction. Rather, there are multiple contributors that are biological, psychological, and social in nature.
Read More
What if a single blood test based on measuring thousands of proteins could provide an accurate portrait of a person’s current health & future disease risks?
Read More
Innovations in dried blood spot testing (DBS) technology will greatly improve the adoption as well as broaden the reach of DBS technology.
Read More
There is an urgent and never-ending need for patient participation in clinical trials, Here are five reasons why you should consider volunteering for one.
Read More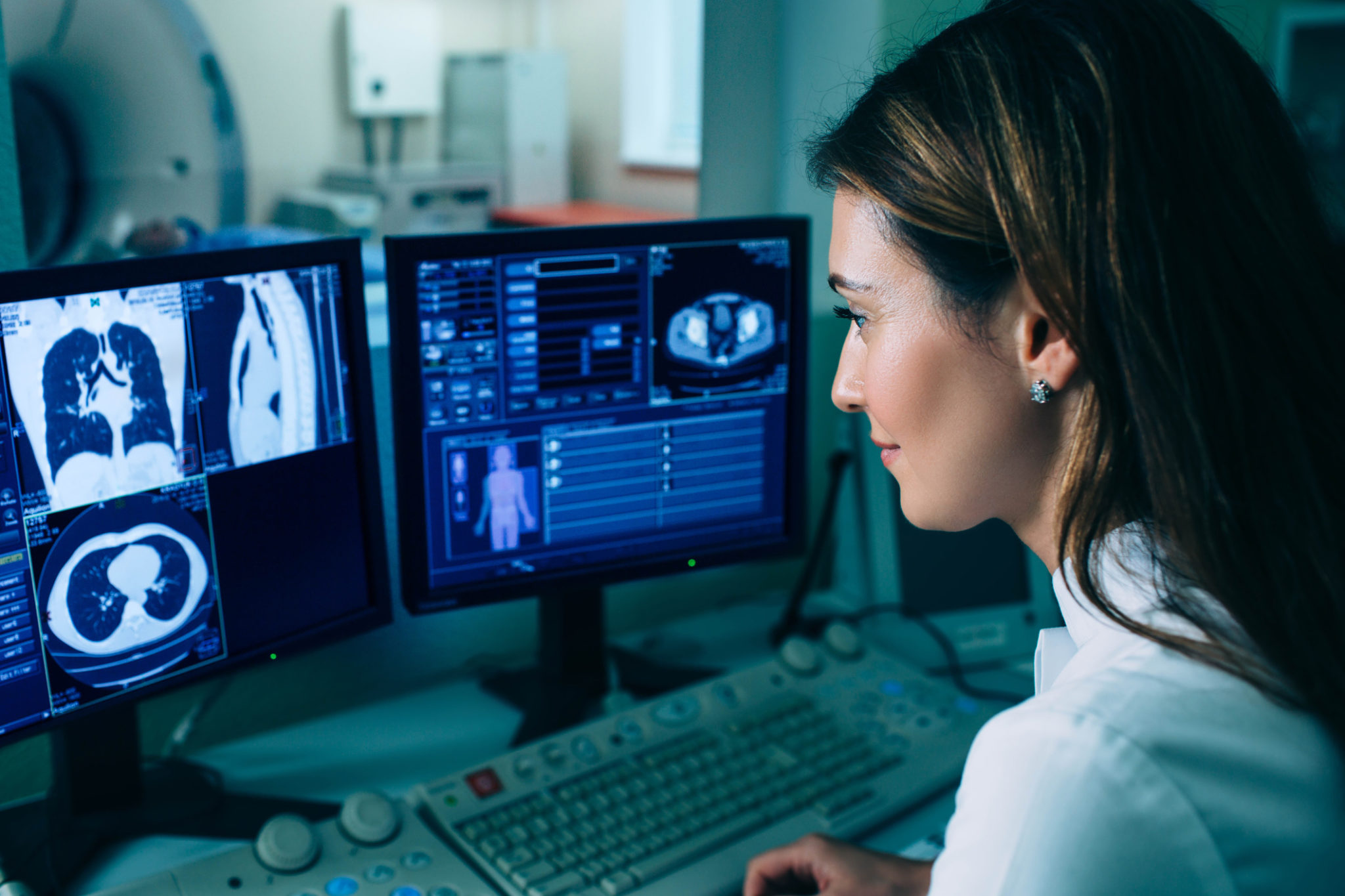
Breast & lung cancer screening programs have led to diagnoses at an earlier stage. AI-deep learning systems improve on those results by reducing diagnostic errors.
Read More
Many people think vision loss is just a normal part of aging but it doesn’t have to be. There are many steps you can take to reduce your risk of blindness.
Read More
The medical community and federal regulators must ensure that risks and benefits of marijuana and CBD being used for medical reasons are properly researched
Read More
Although HLTH did not specifically focus on immune-mediated diseases, a bit of sleuthing uncovered innovations useful for people with those conditions.
Read More
A new survey shows us that patients have a strong desire for their physicians to be involved in helping them with chronic illness management self-care.
Read More