After serendipitously being grouped together during their medical school anatomy class, Shiv Gaglani and Ryan Haynes realized that “the model of medical education is pretty antiquated, even at great schools like Johns Hopkins.” This was the inspiration for their virtual medical education start-up, Osmosis.
That was back in 2012. What they’ve created since then is a web- and mobile-based platform that they believe will help transform the first two years of medical school and health professions training. The total Osmosis package includes videos, flashcards, study schedules, reminders, and more.
Osmosis offers a variety of products including videos, flashcards, reminders, and study scheduling. (Screenshot from the App Store)
In this review, I will focus primarily on Osmosis medical education videos.
Growing Osmosis
Gaglani graduated magna cum laude from Harvard with degrees in engineering and health policy, before enrolling in Johns Hopkins School of Medicine. He also earned an MBA from Harvard Business School in 2016.
Like other medical student entrepreneurs I have met, Gaglani decided to take a leave of absence from medical school to pursue his dream of building what he calls “supplemental online education” for health professional students. That has become the core business of Osmosis.
I had a chance to interview Gaglani, now the company’s CEO about the Osmosis story during the week of the 2019 JP Morgan meetings in San Francisco.
During our discussion, he described the company as “the lead medical education platform dedicated to filling the void of medical learning curriculum…and…the solution for over 850,000 medical students and future healthcare professionals.”
The original focus for the company was medical students, however, the company soon discovered nursing and physician assistant students were watching the educational videos, too. So, they expanded their content to be relevant for dental, pharmacy, nursing and other health professionals as well.
Osmosis is also looking to add postgraduate training modules as well. They expect their first accredited continuing medical education (CME) course (in Cardiology) to go live this year.
Jumpstarting the company
Osmosis got a tremendous boost when the health and medicine team from Khan Academy became available due to a change in strategy. Gaglani explained:
“When the former Khan Academy staff joined they had already made 1500 pre-medical videos. However, the approach that worked for kindergarten through 12th grade and college students was not as effective for health and medicine.”
Even though the new staff was already experienced in making health education videos, Osmosis knew they wanted to vary their approach based on their market research. They knew that the most effective videos required more detail, visual interest, added sound effects, and scripted content.
The decision to accept outside funding also accelerated Osmosis work. Gaglani was initially hesitant to do so, but described the impact of the cash infusion to CrunchBase News:
“What would have taken us three years should only take us by the end of 2019 to complete.”
These decisions, amongst others, has helped propel Osmosis to where they are today. Despite being a relative newcomer to the world of medical education, the platform has already been implemented globally in over 32 universities.
Eleven hundred videos and counting
There are currently more than 1200 videos in the Osmosis library. Three hundred are publicly available for free through YouTube. The rest can be accessed by a subscription either paid by individual professional students or their institutions. Additional features are available only in paid versions include flashcards, notes, and board-style questions.
Videos available via the Osmosis app cover a wide range of topics including:
- Biochemistry
- Cardiovascular
- Cell physiology
- Dermatology
- Embryology
- Endocrine
- Gastrointestinal
- Genetics
- Hematology and oncology
- Immunology
- Microbiology
- Musculoskeletal
- Neurology
- Psychiatry
- Renal
- Reproductive
- Respiratory
As I already mentioned, some of the educational videos are free and others require a subscription. This varies by topic. For example, all but one of the biochemistry videos are behind a paywall but nearly half of the cardiovascular videos are free.
In addition to these general medicine topics, Osmosis also produces videos designed to support students during clinical rotations. Topics include how to work up a patient with anemia, place an IV and more.
Keeping pace with medical advances
One of the greatest challenges for Osmosis is assuring their content is continually updated to keep pace with the knowledge base of medicine. They have developed an approach to meet the need for near-constant revision. They use a whiteboard format and a modular approach that easily allows content updates.
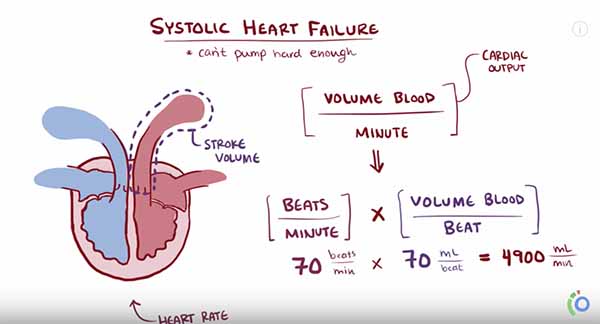
Osmosis uses a whiteboard format to facilitate frequent updates (screenshot from free Osmosis CHF YouTube video)
Gaglani adds they’ve also developed
“a proprietary process for creating videos for low cost and then updating them as well. Like an intron splicing and genetics, we can take out specific parts of the video and replace them with new up-to-date information.”
Videos also generate consumer interest
Just as Osmosis discovered health professionals beyond medical students were watching their videos, they also learned patients and families were watching, too. Although the content was developed for clinicians, many patients and families are often very knowledgeable about their own condition.
The company received a patient comment – in their first month – responding to a clinical video on lupus. Osmosis realized the potential consumer interest in their work.
Patient education videos followed and so did “thousands of comments from patients and family members.”
Consumer-oriented materials are now part of the video mix. It has led to collaborations with many different patient groups. One of the strongest, according to Gaglani, is work they have done with the National Organization for Rare Disorders (NORD), creating videos about rare diseases.

Video explaining maple syrup urine disease, a rare genetic metabolic disorder (screen shot from Osmosis free YouTube video)
Other examples of patient content collaboration include videos on:
- Shared Decision Making (https://www.youtube.com/watch?v=4ueDJEFytMI), Procedures like how to use an inhaler (https://www.youtube.com/watch?v=5gPyNNXP-wA)
- “Knowledge Shots” about topics like smoking vs vaping and CRISPR-Cas9.
What makes a medical video effective?
Through experience and research, Osmosis has discovered that people like a fairly consistent video style. As a result, they use the same illustrator, voiceover artist, etc. for a series.
They are changing things up for the procedural videos adding animation and illustration on top of live footage. A video just produced on IV insertion, intravenous insertions included these new techniques.
Beyond satisfied customers, I asked how Osmosis know their content and approach work. How can you tell if people are learning?
Gaglani admits this a good question. It is one that they are intensely interested in answering. Unlike other consumer tech companies, he said, one can’t just look at the usual metrics such as how much time is spent on the site.
To learn more, the company is conducting research and publishing research papers – 12 so far. They’re looking at usage behavior on Osmosis as well as other metrics of success.
It is important to point out that Osmosis does not rely solely on Board exams scores to determine their outcomes. Gaglani says that, first of all, those results are amongst the hardest to collect. And second, there is also a lot of debate on whether board exams are a good metric for success.
A lot of Osmosis’ research is based on evidence-based education. For example, they are looking at sophisticated areas that relate to accuracy, overconfidence, and calibration. In the clinical context, overconfidence can lead to diagnostic errors while under-confidence can result in defensive medicine.
Osmosis is also analyzing a “whole series of cognitive techniques like spaced repetition, memory palaces, and test-enhanced learning.” They are also doing Institutional Review Board (IRB) approved studies even though they are resource-intense and time-consuming.
How is content developed?
Scriptwriters develop all the Osmosis content. All have medical backgrounds–either a Ph.D. or an MD/Equivalent. And, many actually work for the professional schools who are Osmosis customers. For example, Maureen Richards, an immunology professor at Rush Hospital in Chicago wrote many of the immunology scripts.
Once a script is written, reviewers do an edit. A final review is performed by Rishi Desai, M.D., M.P.H., Osmosis’ Chief Medical Officer. Desai formerly worked at the Khan Academy as Head of Health and Medicine. Prior to that, he was an Epidemiological Intelligence Service (EIS) Officer at the Centers for Disease Control (CDC).
The videos I viewed for professional audiences varied from high-level overviews to more in-depth coverage of the topic. Gaglani stresses, however, that there are two reasons Osmosis doesn’t want to go into too much detail in many of their videos:
“We wanted a baseline level of video that would be accessible. And for globalization and regionalization, treatments differ a lot.”
They add notes to the videos to convey more granular information. And, with their funding and rapid growth, Osmosis is now producing a whole set of videos that are more in-depth to add to their video library.
Reinforcing with retargeting
One unique feature of the Osmosis approach is their ability to track individuals who use the web and mobile-based subscription service whether a video, question or flashcard. According to Gaglani:
“If you watch a video through Osmosis we know who you are and when you watched – unlike watching on YouTube. If you watched a video on hypertension and the guidelines change three years later, we can send you the updated video.”
He adds the ability to do this is “part of why we call it Osmosis – knowledge diffuses to you.”
They also do “retargeting” which he likens to searching Google for a pair of pants and having ads for similar pants follow you even after you leave the original site. Both of these tactics reinforce learning about a topic over time.
Related Content: Leveraging E-Learning for Med Students’ Mental Health
Speeding up medical education
Currently, Osmosis has approximately 30 partnerships with schools. Many are using the platform in a way that allows the faculty to spend less time in the lecture hall for one-hour lectures and more time in the clinic.
This positively impacts institutional resources. It’s also more efficient for students who can choose when to watch educational videos instead of (or in addition to) attending scheduled lectures.
Gaglani believes that Osmosis will have a big impact on the first two years of medical school/health professionals training. He says,
“It is definitely realistic that within a couple of years there will be more schools that will allow you to “test out” of certain courses and go through the curriculum faster.”
Such a change could, among other things, substantially reduce student debt. Two years’ tuition runs $80,000. However, Gagliani notes, accrediting bodies may need to be convinced.
That Osmosis has a broad vision on medical education is underscored by a feature Gaglani calls “TurboTax for test prep.” It’s a daily study schedule that is really popular with students.
Here’s how it works. Let’s say you’re a medical student and plan to take the United States Medical Licensing Examination (USMLE) in three months. The app will walk you through customizing your preferences so that you study in the way you want and still finish the curriculum in the specified time.
For example, you can note that you like to take weekends off. Or whether weekends are actually your preferred study time. You can highlight weak areas that may require more time to learn. Or areas of strength that may require less time. The scheduling feature is available through the Osmosis mobile app. It requires a subscription.
Related content: Innovative Collaboration Can Make Medical School Better
Osmosis Metrics of Success
Osmosis may only be 7 years old, but their numbers are already impressive:
- Revenue has grown 120 percent year-over-year
- 43 remote employees, including contractors
- Over 450,000 registered users
- One psychiatry video has already been viewed over a million times (mental health is popular)
- An audience of over a million on its YouTube channel, tens of thousands of whom are patients
- 75 million views to date
Moreover, the company’s broad vision, wide-ranging partnerships, education, and tech expertise, as well as their commitment to transforming medical education, provides a great foundation for Osmosis to continue to grow their business.
Many thanks to healthcare communication and public affairs consultant, Leslie Rose, for her expert assistance in the preparation of this story.
Patricia Salber, MD, MBA
Website:
https://thedoctorweighsin.com
Patricia Salber, MD, MBA is the Founder. CEO, and Editor-in-Chief of The Doctor Weighs In (TDWI). Founded in 2005 as a single-author blog, it has evolved into a multi-authored, multi-media health information site with a global audience. She has worked hard to ensure that TDWI is a trusted resource for health information on a wide variety of health topics. Moreover, Dr. Salber is widely acknowledged as an important contributor to the health information space, including having been honored by LinkedIn as one of ten Top Voices in Healthcare in both 2017 and 2018.
Dr. Salber has a long list of peer-reviewed publications as well as publications in trade and popular press. She has published two books, the latest being “Connected Health: Improving Care, Safety, and Efficiency with Wearables and IoT solutions. She has hosted podcasts and video interviews with many well-known healthcare experts and innovators. Spreading the word about health and healthcare innovation is her passion.
She attended the University of California Berkeley for her undergraduate and graduate studies and UC San Francisco for medical school, internal medicine residency, and endocrine fellowship. She also completed a Pew Fellowship in Health Policy at the affiliated Institute for Health Policy Studies. She earned an MBA with a health focus at the University of California Irvine.
She joined Kaiser Permanente (KP)where she practiced emergency medicine as a board-certified internist and emergency physician before moving into administration. She served as the first Physician Director for National Accounts at the Permanente Federation. And, also served as the lead on a dedicated Kaiser Permanente-General Motors team to help GM with its managed care strategy. GM was the largest private purchaser of healthcare in the world at that time. After leaving KP, she worked as a physician executive in a number of health plans, including serving as EVP and Chief Medical Officer at Universal American.
She consults and/or advises a wide variety of organizations including digital start-ups such as CliniOps, My Safety Nest, and Doctor Base (acquired). She currently consults with Duty First Consulting as well as Faegre, Drinker, Biddle, and Reath, LLP.
Pat serves on the Board of Trustees of MedShare, a global humanitarian organization. She chairs the organization’s Development Committee and she also chairs MedShare's Western Regional Council.
Dr. Salber is married and lives with her husband and dog in beautiful Marin County in California. She has three grown children and two granddaughters with whom she loves to travel.

















Comment will held for moderation