There’s an old saying: “I didn’t skip a beat.” But sometimes, we do.
As more and more people are using commercially available wearable rhythm monitoring devices to track their health, many discover that they sometimes have an irregular, slow or very fast heart rate.
Wearable heart rhythm monitoring devices are typically worn on the wrist or on a chest strap. Many contain smart sensors that can record both heart rate and rhythm. The devices can connect to the internet for data reporting.
Walkers, runners, cyclists, swimmers, and people who simply want to track or improve their level of fitness increasingly use wearable devices, including those that monitor heart rhythm. In fact, the research firm CCS Insight reports that global sales of smart wearable devices are predicted to double between 2018 and 2022 to 233 million units.[i]
Let me preface the rest of my remarks by saying that when people detect skipped beats, rapid heart rates, slow heart rates, or other potential heart issues using their wearables, they should see a physician to learn what is causing their problem and whether it needs to be treated.
What Skipped, Slow, or Rapid Heart Beats May Mean
A “cardiac arrhythmia” is an abnormal heart rhythm that typically develops when disease or injury disrupts the heart’s electrical signals, causing the heart to beat erratically. Sometimes it’s slow and sometimes it’s fast.
In some cases, it is associated with and/or causes symptoms such as fainting, passing out or feeling short of breath. Other times people simply feel heart palpitations or dizziness.
Some arrhythmias are specifically associated with an increased risk of stroke, such as atrial fibrillation, or AFib, a condition in which the upper chambers of the heart beat very rapidly and erratically, and quiver or “fibrillate.”
This condition is the most common abnormal heart rhythm seen in clinical practice. The risk for AFib increases with age. Since people are living longer, there has been a surge in the world’s aging population that has contributed to the rise of AFib around the globe. As many as 6.1 million people in the United States alone are affected by AFib.[ii]
People often notice they have a heart rhythm issue either through their wearable device or because of symptoms, resulting in a trip to their physician.
But the chance of capturing the problem in the physician’s office is relatively low. So, the physician may order a traditional Holter monitor or a remote rhythm monitoring device that is implanted just under the skin to help confirm the underlying problem.
Since irregularities in a person’s heart rhythm can come and go unpredictably, remote monitoring plays an important role in diagnosis and determining a treatment path for these individuals.
Basic Monitoring as the First Step
Wearable devices play an important role in improving fitness and alerting users to potential health issues, such as irregular heartbeats.
The increased popularity and sophistication of wearable devices means these products are a good first step in identifying an arrhythmia or anomaly that might have gone undetected before.
Wearable devices have certain inherent limitations when it comes to making a clinical diagnosis. These include requiring removal at night for recharging and generally recording only a single-lead (one connection) electrocardiogram (ECG).
Related: How to Mitigate the Risks of Remote patient monitoring.
Additionally, heart rhythm issues happen sporadically, and most people do not wear their devices all day, every day.
Traditional Holter monitoring
Once a physician is alerted to a potential cardiac rhythm issue, they often prefer to monitor with an approved medical device such as a traditional Holter monitoring device.
These battery-operated devices are about the size of a postcard. The patient usually wears it via a strap around the neck or an elastic band around the waist. There are EKG leads that attach to the chest.

Photo source: Adobe stock photo
The device collects data recorded from the ECG continuously for a given time. Typically, it is used anywhere from 48 hours to a week or more.
The challenge with Holter monitors is that they can be cumbersome and delay important treatment. Patients must return the device to the doctor’s office.
Then, the doctor must download and analyze the data before meeting again with the patient to discuss the results.
If the problem isn’t detected during this monitoring period, the cardiologist may prescribe additional time wearing the Holter. Or he may prescribe an implantable continuous remote monitoring device instead.
Continuous Remote Heart Monitoring
The use of an implantable continuous heart monitor provides several benefits:
- Insertable cardiac monitors record heart activity continuously. They can pick up potentially dangerous heart rhythm problems (arrhythmias) over an extended amount of time. This can range from weeks to months or even a couple of years.
- These devices can transmit data directly to a physician’s office on a daily basis to identify an irregularity as soon as it happens. In fact, new monitors can transmit data via smartphone. Healthcare providers then evaluate the data and can follow up immediately.
Abbott’s Confirm Rx™ ICM System
One option for insertable cardiac monitoring is Abbott’s Confirm Rx™ ICM system. It is the world’s first continuous heart monitor that is smartphone compatible.
The system monitors a patient’s heart rhythm around the clock. The device automatically transmits the data every night simply by being in the range of the user’s smartphone that is connected to Bluetooth and the internet.
There’s no need for additional monitoring equipment or a recharging station. There is also no need to rely on the patient to take action.
However, patients can also flag issues or symptoms as they experience them and transmit the episode immediately.
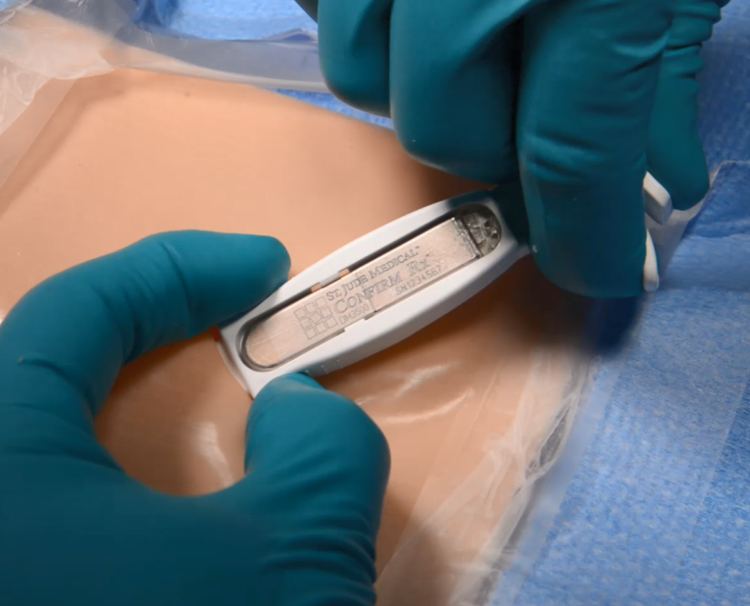
Insertion of the Abbott Confirm Rx device
Photo courtesy of Abbott
These insertable cardiac monitors are small – around the size of a paper clip. They are implanted under the skin during a quick outpatient procedure using a local anesthetic. No sutures are required and there is usually only minimal scarring.
The Future of Remote Monitoring
As advances in wearable technology continue, remote monitoring is likely to evolve, as well. For example, data from a variety of devices will likely be fully integrated instead of just shared.
Related: Is the Future of American Healthcare Digital?
Soon we may be able to monitor and record physical or psychological signals that can affect such things as blood pressure, heart rate, insulin levels, stomach acid, and asthma.
As we learn more about the importance of these types of biological signals, we will become better at correlating sensations and symptoms with biological data.
While these advancements represent benchmarks in innovation, each one moves us closer to helping improve outcomes for patients around the world.
References
[i] CSS Insight. Success of Apple Watch Means More Growth in Sales of Wearable Technology https://www.ccsinsight.com/press/company-news/3695-success-of-apple-watch-means-more-growth-in-sales-of-wearable-technology. Accessed January 23, 2019.
[ii] Mozaffarian D, Benjamin EJ, Go AS, Arnett DK, Blaha MJ, Cushman M, et al. Heart disease and stroke statistics—2015 update: a report from the American Heart Association. Circulation. 2015;131:e29–e322.
Avi Fischer, M.D.
Avi Fischer is Divisional Vice President, Medical Affairs and Medical Director for Cardiac Rhythm Management (CRM) within Abbott Cardiac Arrhythmias and Heart Failure. Prior to this position, as Vice President of Global Education, Avi led a global team responsible for customer and employee education and training across all products and therapies for St. Jude Medical. Avi joined St. Jude Medical in June 2012, serving as Vice President, Medical Affairs and Medical Director for the St. Jude Medical Implantable Electronic Systems Division. Dr. Fischer received an undergraduate degree from the University of Maryland and an M.D. from the Sackler School of Medicine, Tel Aviv University. He completed residency training in Internal Medicine at The Albert Einstein School of Medicine, Montefiore Medical Center and then completed a fellowship in Cardiovascular Diseases at the Mount Sinai School of Medicine and a fellowship in Clinical Cardiac Electrophysiology at the Brigham and Women’s Hospital, Harvard University. He joined the faculty of the Mount Sinai School of Medicine in 2006 as Director of Pacemaker and Defibrillator therapy. Avi is a fellow of the American College of Cardiology and the Heart Rhythm Society and has participated in numerous ACC and HRS societal committees on cardiac implantable electronic devices and quality initiatives. He has been a member of the invited faculty at international scientific congresses and has trained and proctored physicians around the world on lead management and lead extraction. Dr. Fischer has authored numerous original publications, invited reviews and book chapters.









Comment will held for moderation